 Kris Gladwell, MHCF President & CEO Kris Gladwell, MHCF President & CEO It has been just over one year since I joined the MHC family as President & CEO of the MHC Foundation – and what a year it has been! While I had hoped to meet many of you in person at our 2020 events – such as the Golf Classic, Gala, and Angel Squad – obviously, COVID-19 drastically altered those plans. However, this past year has allowed me to learn about the MHC donor family in an incredibly meaningful way. Thank you. Since the onset of the pandemic, the outpouring of generosity you have shown to Misericordia has been touching and incredibly appreciated. All the messages of support for our health-care heroes have been passed along to them, and your donations have ensured they have continuously remained nourished – physically and emotionally. Your support brings virtual care to MHC by providing new technology and ensuring patients and residents remain connected to their loved ones, preventing social isolation with enhanced programing and services. Your support also helps MHC visitors feel safe as they walk through the halls in the medical-grade masks supplied to them. Please know your generosity at every level is having a tremendous impact on the incredible work taking place at MHC each and every day. On behalf of everyone who has benefited from your support over the last year, thank you. We are beyond grateful. Whatever lies ahead, you can rest assured that MHC’s commitment to providing exceptional and compassionate care will never waver. Thanks to the generosity of donors like you, those on the front lines will continue enhancing patient experiences by incorporating the latest and best practices to re-envision the future of care. As MHC evolves to meet the health-care needs of our community, I am so honoured to lead the Foundation through this exciting time. I invite you to continue to follow Misericordia’s story. We look forward to connecting with you regularly through our MHC Moments e-newsletter, and you can always see what we are up to on social media. Please join us on Facebook, Instagram, LinkedIn, and Twitter! Thank you for being a part of the MHC Foundation family. With gratitude, Kris
1 Comment
[Editor's note: Our OR nurses, Yvonne & Colleen (profiled below), were among the more than 30 MHC staff who were redeployed to work in ICUs and acute care at other hospitals during the third wave of COVID-19. Click here to read more about the impact of COVID-19 on MHC.] 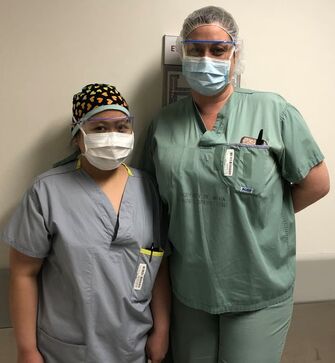 Yvonne (left) and Colleen (right) Yvonne (left) and Colleen (right) During the first wave of the pandemic, members of the operating room (OR) team were reassigned to other program areas at Misericordia, including Colleen Kunderman, registered nurse (RN), who spent two months answering calls on the Health Links – Info Santé COVID-19 line. “During the second wave, I assumed I might be redeployed to another site,” said Colleen over the phone after working the night shift on Cornish 6, a transitional care unit at MHC. “It was nice to stay on-site at MHC – it’s familiar.” Yvonne Mendoza, RN, is an OR team member who in mid-November, like Colleen, was reassigned to transitional care. “At first I was scared. I thought the change would be overwhelming,” said Yvonne candidly. She continued: “But I remembered that I would bloom where I was planted, because I was there for a reason.” Colleen and Yvonne both spent some time over at Misericordia Place, but primarily worked on Cornish 6 (C6) and Cornish 5 (C5) transitional care units, respectively, for the past two months. With their reassignment came big changes both professionally and personally. Both RNs were accustomed to working eight-hour shifts, Monday to Friday, as well as being on call, and had to adjust to working 12-hour shifts, days, evenings as well as sometimes working seven days on. However, the biggest changes came with the new roles themselves. “In the OR, my interactions with patients were limited to usually five minutes or less. On C6, it’s continual patient care, so my duties included: assessment and taking vitals, administering meds, assisting with feeding and transfers, helping patients FaceTime their families, really everything but admin,” said Colleen. Yvonne, who was reassigned to entrance screening during the first wave of the pandemic, expressed that in moving from the OR to C5, the systems and processes are different, incomparable. “At the end of the day, it was very satisfying working on C5. I learned so many new things with the help of the C5 team – they’re amazing and very supportive,” said Yvonne. With visitation restrictions in place in order to protect patients and residents and help halt the spread of COVID-19, health-care providers are important sources of support and meaningful interaction for clients and residents. “We all have had our difficult moments during COVID. But nothing compares to the experience that some patients and residents have had. They’ve lost spouses and couldn’t attend funerals. They haven’t seen family members in person for months on end. Throughout my experience on C6, it made me see that there was a real need and purpose for me – and my colleagues – in being reassigned.” Colleen and Yvonne have now returned to their usual roles in the OR. To both of these health-care heroes and their colleagues, thank you for helping where needed most at MHC. To support MHC health-care heroes like Yvonne and Colleen, please make your gift today! |
have a story to share?We'd love to hear it!
Share your story Categories
All
|
|
Misericordia Health Centre Foundation 99 Cornish Avenue Winnipeg, MB, Canada R3C 1A2 Tel: 204-788-8458 Fax: 204-774-0766 mhcfoundation@misericordia.mb.ca Charitable Registration Number: 11904 2174 RR0001 |
|


